Introduction
Sleep is essential for physical health, mental clarity, and emotional wellbeing. Yet, many people struggle with persistent fatigue, snoring, or unexplained daytime sleepiness. A professional sleep study, also known as a sleep test, can help identify underlying sleep disorders that may be affecting your health. Understanding the signs that indicate a sleep study is needed can help you take proactive steps toward better rest and overall wellbeing.
What is a Sleep Test?
A sleep test monitors your body’s activity while you sleep to detect potential disorders. It provides detailed information about:
- Brain activity (EEG) for sleep stages
- Eye movements to identify REM sleep
- Heart rate and rhythm
- Breathing patterns and oxygen levels
- Muscle activity and limb movements
These metrics help diagnose conditions such as obstructive sleep apnoea, insomnia, restless leg syndrome, and narcolepsy, allowing for accurate treatment plans.
Signs You May Need a Sleep Study
Certain symptoms can indicate that a sleep test may be beneficial:
1. Persistent Daytime Sleepiness
- Feeling excessively tired despite adequate hours of sleep
- Struggling to stay awake during work, school, or driving
- Regularly relying on caffeine or naps to stay alert
2. Loud or Frequent Snoring
- Snoring that disrupts your own or your partner’s sleep
- Pauses in breathing during sleep, choking, or gasping
3. Difficulty Falling or Staying Asleep
- Trouble initiating sleep or waking up frequently
- Feeling unrested despite a full night’s sleep
4. Unusual Movements or Sensations
- Twitching, jerking, or restless leg movements
- Nighttime teeth grinding or other repetitive behaviours
5. Morning Headaches or Poor Concentration
- Waking with headaches, dry mouth, or sore throat
- Difficulty focusing, memory problems, or irritability
If you notice one or more of these signs consistently, a sleep study may be necessary to determine the cause.
Preparing for Your First Sleep Study
Proper preparation can make your first study more comfortable and effective:
- Maintain a consistent sleep schedule in the days leading up to the study
- Avoid caffeine, alcohol, or sedatives on the day of the test
- Wear comfortable, loose-fitting pyjamas
- Bring personal comfort items, such as a pillow or blanket
- Follow any specific instructions from your sleep clinic, including medication guidance
In-Lab vs Home Sleep Studies
In-Lab Polysomnography (PSG)
- Conducted overnight in a clinic with specialised equipment
- Monitors brain, heart, breathing, oxygen, and limb movements
- Supervised by trained sleep technicians
- Recommended for complex or unclear sleep disorders
Home Sleep Tests
- Conducted in the comfort of your own bed
- Focuses on breathing, heart rate, and oxygen levels
- Simple setup and remote guidance from a sleep specialist
- Suitable for suspected sleep apnoea or routine monitoring
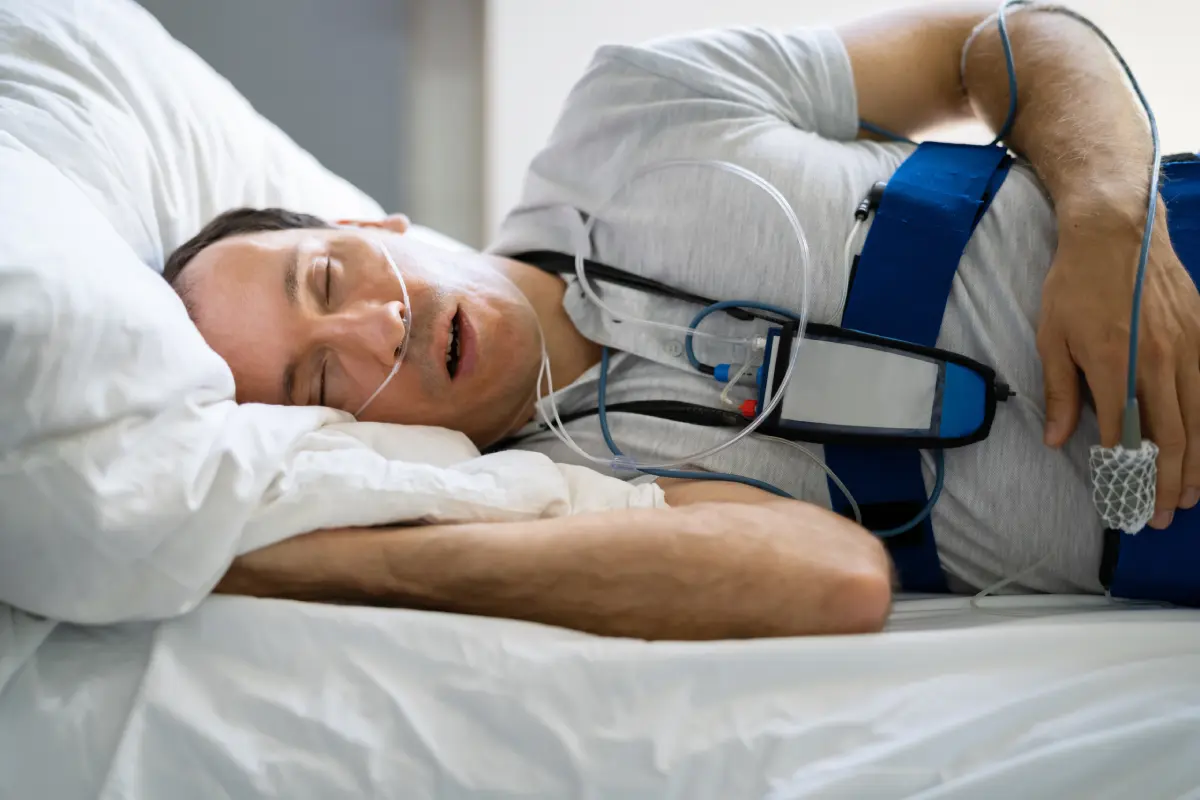
What to Expect During the Night
- Sensors and electrodes attached to the head, chest, and limbs
- Breathing and oxygen monitoring through a nasal cannula and fingertip sensor
- Minimal intrusion: modern equipment is lightweight and comfortable
- Observation and reassurance: technicians may monitor you remotely in home tests or stay nearby in-lab
The goal is to capture natural sleep patterns while ensuring safety and comfort.
How Sleep Test Results Are Used

Key metrics help specialists determine appropriate interventions:
- Apnoea-Hypopnoea Index (AHI): Measures breathing interruptions per hour
- Oxygen desaturation levels: Identifies drops in blood oxygen
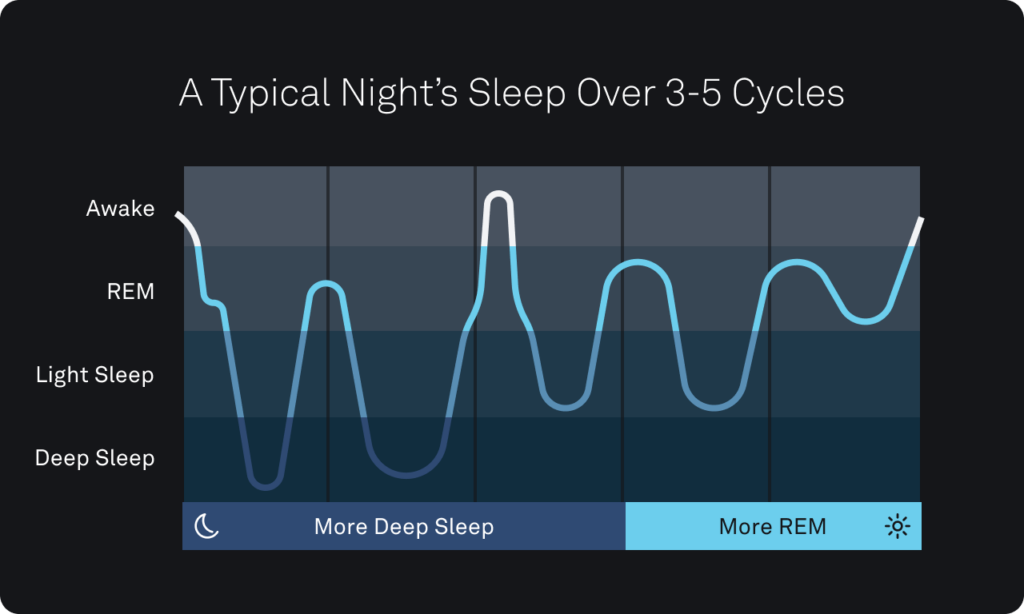
- Sleep stage distribution: Balances of REM and NREM sleep
- Heart rate and rhythm: Detects cardiovascular risks
- Limb movements: Indicates conditions like restless leg syndrome
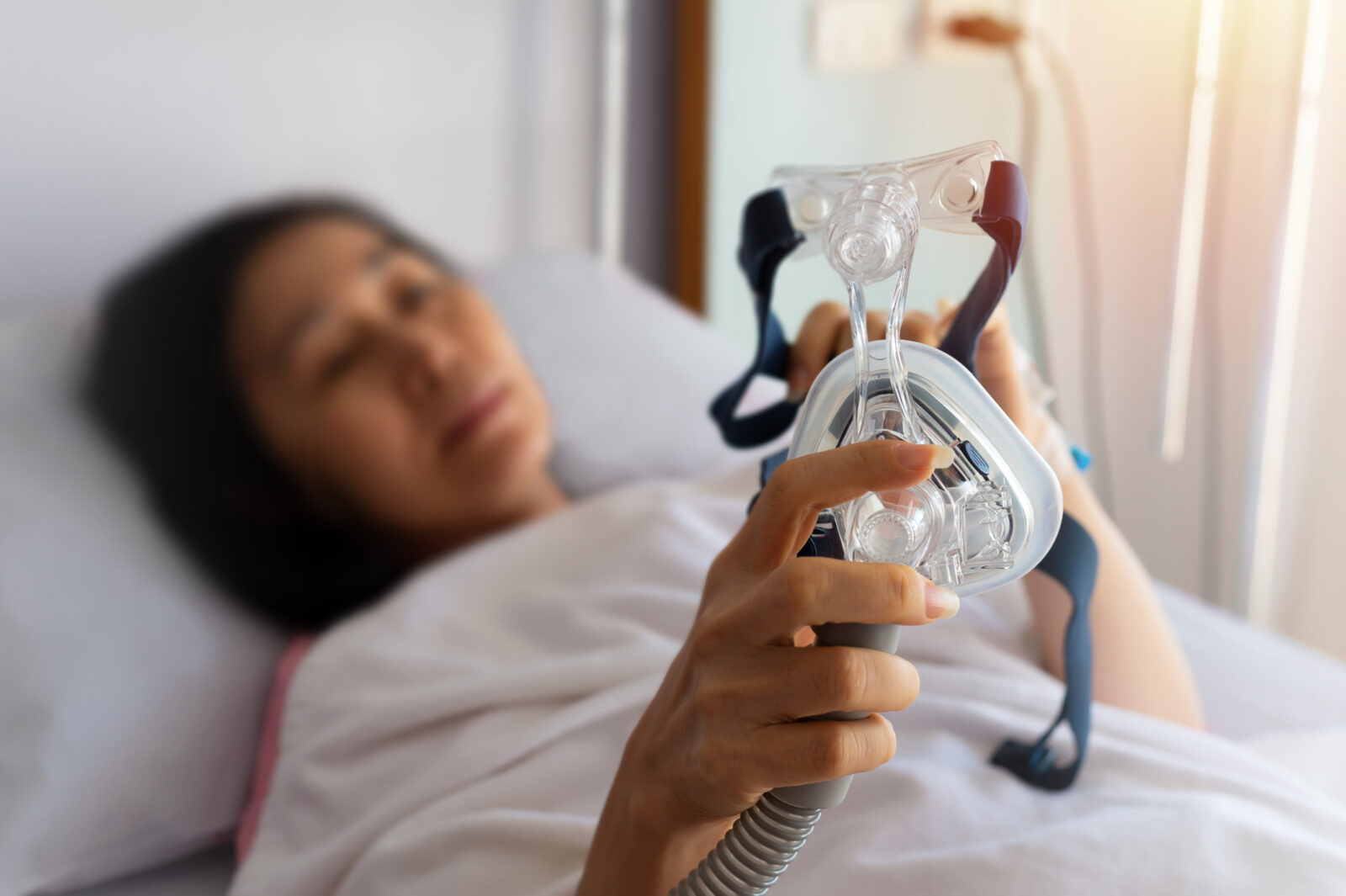
Using these results, doctors can recommend targeted treatments such as CPAP therapy, lifestyle adjustments, medications, or behavioural interventions.
Benefits and Potential Discomforts
Benefits
- Identifies sleep disorders accurately
- Improves sleep quality and daytime energy
- Reduces health risks associated with poor sleep
- Provides guidance for long-term sleep health
Potential Discomforts
- Mild skin irritation from electrodes
- Nasal or facial discomfort from sensors
- Initial sleep disruption due to unfamiliar equipment
Modern sleep tests are far more comfortable and less intrusive than older methods, making the experience manageable for most patients.
Patient Experiences
- “I was sceptical, but the sleep study explained why I was always exhausted. CPAP therapy has made a huge difference.”
- “The home study was easy to set up, and the results guided my doctor in treating my sleep apnoea effectively.”
- “Understanding my sleep patterns gave me peace of mind and helped me prioritise better sleep habits.”
These experiences highlight the importance of recognising symptoms and taking proactive steps.
Conclusion
If you experience persistent fatigue, snoring, sleep disturbances, or unusual movements at night, a professional sleep study may be the key to uncovering underlying sleep disorders. With proper preparation and guidance from specialists, sleep tests can provide crucial insights, allowing for personalised treatment plans that improve sleep quality, daytime energy, and overall health.
FAQs
1. How do I know if I need a sleep study?
If you experience persistent fatigue, loud snoring, breathing pauses, restless sleep, or difficulty concentrating, a sleep study may be needed. Specialists use these symptoms to decide the type of study and ensure accurate diagnosis.
2. Are home sleep tests as reliable as in-lab studies?
Yes, for most patients with suspected sleep apnoea, home tests are accurate and convenient. In-lab studies provide more detailed data and are preferred for complex or unclear cases.
3. What should I do to prepare for a sleep study?
Maintain a regular sleep schedule, avoid caffeine or alcohol, wear comfortable clothing, and bring personal comfort items. Follow any specific instructions from your sleep clinic regarding medications or bedtime routines.
4. What discomforts might I experience during a sleep study?
Minor skin irritation from electrodes, nasal or facial discomfort from sensors, and slight sleep disruption may occur. Modern equipment is lightweight and designed for patient comfort.
5. How do sleep test results improve health?
Results identify sleep disorders, guide personalised treatments like CPAP therapy or lifestyle changes, improve sleep quality, reduce daytime fatigue, and lower long-term health risks associated with poor sleep.