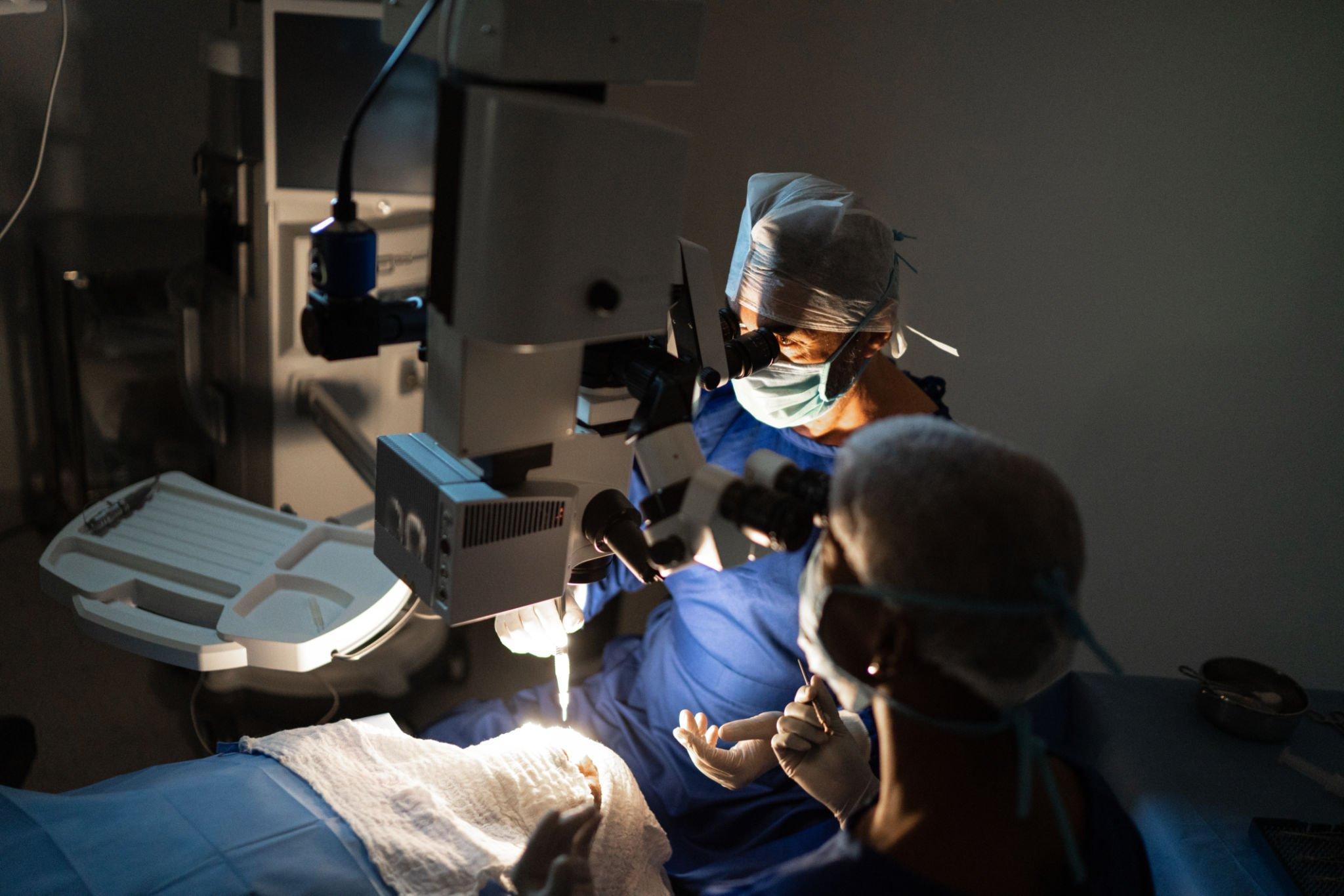
Glaucoma is a condition that affects the optic nerve, causing gradual vision loss if left untreated. While there are different treatment options available for glaucoma, surgery is often recommended in cases where medication or other non-invasive measures have not been effective.
In this article, we will explore the different types of glaucoma eye surgery and provide an overview of each procedure to help you understand which one may be right for you.
Understanding Glaucoma
Glaucoma is an eye disease characterized by damage to the optic nerve, which is responsible for transmitting visual information from the eye to the brain. This condition is typically caused by increased pressure within the eye, known as intraocular pressure.
Glaucoma is a complex disease that affects millions of people worldwide. It is often referred to as the “silent thief of sight” because it can progress slowly and without noticeable symptoms until significant vision loss occurs. Understanding the causes and symptoms of glaucoma is crucial for early detection and treatment. Click here for overview minimally invasive glaucoma surgery (MIGS).
Causes of Glaucoma
The exact causes of glaucoma are not always known, but several risk factors have been identified. One of the primary risk factors is a family history of glaucoma. If you have a close relative, such as a parent or sibling, with glaucoma, you may be at a higher risk of developing the disease.
Advanced age is another significant risk factor for glaucoma. As we get older, our risk of developing the disease increases. It is essential for individuals over the age of 40 to have regular eye exams to monitor their eye health and detect any signs of glaucoma.
In addition to family history and age, certain medical conditions can increase the risk of glaucoma. People with diabetes, for example, are more likely to develop glaucoma due to changes in blood flow and increased pressure within the eye. Other medical conditions, such as high blood pressure and heart disease, can also contribute to the development of glaucoma.
Furthermore, long-term use of corticosteroid medications, such as prednisone, can increase the risk of glaucoma. These medications are commonly prescribed for various conditions, including asthma, arthritis, and certain autoimmune disorders. If you are taking corticosteroids, it is essential to discuss the potential risks with your healthcare provider and have regular eye exams to monitor your eye health.
Symptoms of Glaucoma
Glaucoma can present with different symptoms depending on the type and stage of the disease. However, it is important to note that in the early stages, glaucoma may not cause any noticeable symptoms, which is why regular eye exams are crucial for early detection.
One of the most common symptoms of glaucoma is a gradual loss of peripheral vision. This means that over time, you may notice a decrease in your ability to see objects or people on the sides of your visual field. This symptom often goes unnoticed until it becomes more severe.
In some cases, glaucoma can also cause blurred vision. You may find it challenging to focus on objects or notice a general haziness in your vision. This symptom can be intermittent and may worsen over time if left untreated.
Eye pain or redness can also occur in some individuals with glaucoma. This is typically associated with acute angle-closure glaucoma, a less common but more severe form of the disease. If you experience sudden eye pain, redness, or a sudden decrease in vision, it is essential to seek immediate medical attention.
It is important to remember that glaucoma is a progressive disease, meaning it worsens over time if left untreated. Regular eye exams, especially for individuals at higher risk, can help detect glaucoma in its early stages when treatment options are most effective.
The Importance of Early Detection
Early detection is crucial in managing glaucoma. It allows for timely intervention and treatment, which can help prevent or slow down the progression of the disease. Glaucoma is often referred to as the “silent thief of sight” because it typically does not cause noticeable symptoms until it has already caused significant damage to the optic nerve.
Regular eye exams play a vital role in the early detection of glaucoma. These exams are not only important for assessing visual acuity but also for identifying potential eye diseases, including glaucoma. Comprehensive screenings for glaucoma involve a series of tests and evaluations that can help detect the condition in its early stages.
Regular Eye Exams and Glaucoma
During a comprehensive eye exam, the eye care professional will measure the intraocular pressure (IOP) using a tonometer. Elevated IOP is one of the primary indicators of glaucoma. By measuring the pressure inside the eye, the eye care professional can assess the risk of developing glaucoma and determine the appropriate course of action.
In addition to measuring IOP, the eye care professional will examine the optic nerve. The optic nerve is responsible for transmitting visual information from the eye to the brain. In glaucoma, the optic nerve becomes damaged over time due to increased pressure inside the eye. By carefully examining the optic nerve, the eye care professional can identify any signs of glaucoma-related damage.
Assessing peripheral vision is another crucial aspect of glaucoma screenings. Glaucoma often affects peripheral vision first, causing blind spots or tunnel vision. By conducting a visual field test, the eye care professional can detect any abnormalities in the patient’s peripheral vision, which may indicate the presence of glaucoma.
Risk Factors for Glaucoma
Understanding the risk factors associated with glaucoma is essential for individuals to recognize their potential susceptibility to the condition. While anyone can develop glaucoma, certain factors increase the risk:
- Age: The risk of developing glaucoma increases with age, especially after the age of 60.
- Family History: Having a close relative with glaucoma, such as a parent or sibling, increases the risk.
- Medical Conditions: Certain medical conditions, such as diabetes, high blood pressure, and heart disease, are associated with an increased risk of glaucoma.
- Ethnicity: People of African, Hispanic, and Asian descent are more prone to developing certain types of glaucoma.
- Eye Health: Certain eye conditions, such as high myopia (nearsightedness) or previous eye injuries, can increase the risk of glaucoma.
Recognizing these risk factors can prompt individuals to seek regular screenings to ensure early detection and appropriate treatment if necessary. Early intervention can help preserve vision and prevent the progression of glaucoma-related vision loss.
Overview of Glaucoma Surgery
The Role of Surgery in Glaucoma Treatment
Glaucoma surgery is typically considered when other treatment options, such as medication or laser therapy, have not adequately controlled intraocular pressure. The primary goal of glaucoma surgery is to lower the pressure within the eye and preserve or improve vision.
Glaucoma is a chronic eye condition that can lead to irreversible vision loss if left untreated. It is caused by a buildup of fluid in the eye, which increases the pressure inside the eye. This increased pressure can damage the optic nerve, leading to vision loss.
While medication and laser therapy are often the first line of treatment for glaucoma, they may not always be sufficient in controlling the intraocular pressure. In such cases, glaucoma surgery becomes necessary to prevent further damage to the optic nerve and preserve vision.
There are different types of glaucoma surgery, each with its own benefits and risks. The choice of surgery depends on various factors, including the severity of the glaucoma, the patient’s overall health, and the surgeon’s expertise.
Preparing for Glaucoma Surgery
Prior to undergoing glaucoma surgery, your eye doctor will evaluate the severity of your condition and determine the most suitable surgical approach for your specific needs. Preoperative preparations may include further diagnostic tests, discussions about potential risks and benefits, and instructions to follow before the surgery.
During the preoperative evaluation, your eye doctor will perform a comprehensive eye examination to assess the extent of the glaucoma and evaluate the overall health of your eyes. This may involve measuring the intraocular pressure, examining the optic nerve, and assessing the visual field.
Based on the results of these tests, your eye doctor will discuss the different surgical options available to you. They will explain the potential risks and benefits associated with each procedure, allowing you to make an informed decision about your treatment.
In addition to discussing the surgical options, your eye doctor will provide you with detailed instructions on how to prepare for the surgery. This may include guidelines on fasting before the procedure, discontinuing certain medications, and arranging for transportation to and from the surgical facility.
It is important to follow these instructions carefully to ensure the success of the surgery and minimize the risk of complications. Your eye doctor may also prescribe medications or eye drops to be used before the surgery to help prepare the eye for the procedure.
Furthermore, it is essential to inform your eye doctor about any underlying medical conditions or allergies you may have, as well as any medications you are currently taking. This will help them tailor the surgical approach to your specific needs and minimize the risk of adverse reactions.
Overall, the preoperative preparation phase is crucial in ensuring a safe and successful glaucoma surgery. By carefully following your eye doctor’s instructions and addressing any concerns or questions you may have, you can help optimize the outcome of the procedure and improve your chances of preserving or improving your vision.
Different Types of Glaucoma Surgery
Trabeculectomy
Trabeculectomy is a surgical procedure commonly used to treat glaucoma. It involves creating a small incision in the sclera, the white part of the eye, to allow excess fluid to drain out of the eye and reduce intraocular pressure. A small flap is then created to cover the incision, helping to regulate the flow of fluid.
Laser Trabeculoplasty
Laser trabeculoplasty is a non-invasive surgical procedure that uses laser energy to improve the drainage of fluid from the eye. During the procedure, a laser is focused on the drainage angle of the eye to clear blockages and facilitate fluid outflow, resulting in reduced intraocular pressure.
Minimally Invasive Glaucoma Surgery (MIGS)
Minimally invasive glaucoma surgery, or MIGS, refers to a group of surgical procedures that offer a less invasive alternative to traditional glaucoma surgeries. These procedures typically involve the insertion of tiny stents or implants to improve the drainage of fluid from the eye and reduce intraocular pressure.
Choosing the Right Procedure
Factors to Consider
When determining the most appropriate glaucoma surgery for an individual, several factors need to be considered. These factors may include the severity of the glaucoma, the individual’s overall health, the presence of other eye conditions, and the patient’s preferences and expectations regarding the surgical outcome.
Discussing Options with Your Doctor
Choosing the right glaucoma surgery requires a thorough discussion with your eye doctor or ophthalmologist. They will evaluate your specific circumstances, explain the benefits and risks associated with each procedure, and help you make an informed decision that aligns with your individual needs and goals.
In conclusion, glaucoma surgery plays a crucial role in managing the condition and preventing vision loss. Understanding the different types of glaucoma surgery and considering the individual factors involved can help determine the most suitable procedure for each patient. If you are experiencing symptoms of glaucoma or have been diagnosed with the condition, it is essential to consult with your eye doctor to explore the surgical options available to you.