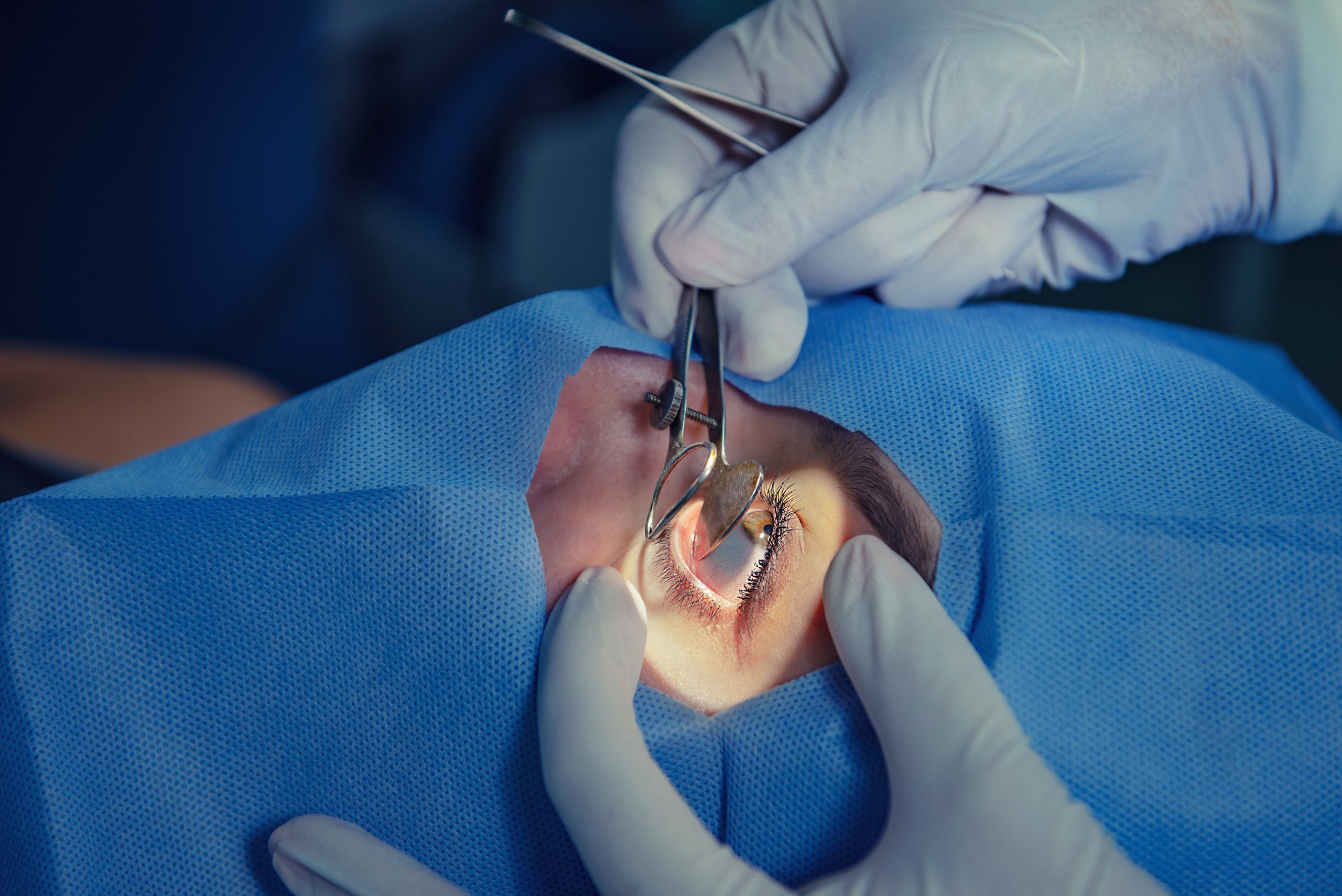
Glaucoma is a complex eye disease that affects millions of people worldwide. It is characterized by the damage to the optic nerve, leading to progressive vision loss over time. There are various treatment options available for glaucoma, including medication and surgery. One innovative approach that has gained popularity in recent years is Minimally Invasive Glaucoma Surgery (MIGS).
Understanding Glaucoma
Before delving into MIGS, it’s important to have a basic understanding of glaucoma symptoms floaters. Glaucoma occurs when there is a buildup of fluid in the eye, resulting in increased intraocular pressure (IOP). This elevated pressure puts stress on the optic nerve, causing damage and vision loss. Glaucoma is often a silent disease, as it progresses slowly and with minimal or no symptoms in the early stages.
Glaucoma is a complex eye condition that affects millions of people worldwide. It is a leading cause of irreversible blindness, making it crucial to raise awareness and educate individuals about its nature, risk factors, and symptoms. Learn more types of glaucoma surgery.
The Nature of Glaucoma
Glaucoma can be broadly classified into two types: open-angle glaucoma and angle-closure glaucoma. Open-angle glaucoma is the most common form, accounting for about 90% of all cases. It develops gradually and is characterized by a gradual clogging of the drainage canals in the eye, leading to increased IOP.
The drainage canals, known as the trabecular meshwork, play a vital role in maintaining the balance of fluid in the eye. When these canals become blocked or clogged, the fluid cannot flow out properly, resulting in a buildup of pressure. This increased intraocular pressure can cause damage to the optic nerve, leading to vision loss over time.
Angle-closure glaucoma, on the other hand, is less common but more severe. It occurs when the drainage canals become blocked suddenly, causing a rapid rise in IOP. This type of glaucoma requires immediate medical attention as it can lead to a sudden and painful increase in intraocular pressure, causing severe damage to the optic nerve and potentially permanent vision loss.
Risk Factors and Symptoms
Several risk factors are associated with the development of glaucoma. Age is a significant risk factor, as the likelihood of developing glaucoma increases with age. Individuals over the age of 60 are at a higher risk. Additionally, individuals with a family history of glaucoma are more likely to develop the condition themselves.
Ethnicity also plays a role in glaucoma risk. People of African, Asian, and Hispanic descent are more prone to developing certain types of glaucoma. Other medical conditions, such as high blood pressure and diabetes, can also increase the risk of glaucoma.
While glaucoma may not produce noticeable symptoms in the early stages, as it progresses, individuals may experience vision loss, blurred vision, eye pain, headaches, and halos around lights. These symptoms can significantly impact a person’s quality of life and should not be ignored.
Regular eye exams are crucial for early detection and timely treatment of glaucoma. During an eye exam, an ophthalmologist can measure the intraocular pressure, examine the optic nerve, and assess the overall health of the eyes. Early diagnosis and intervention can help slow down the progression of glaucoma and preserve vision.
In conclusion, glaucoma is a complex eye condition that requires a comprehensive understanding to effectively manage and treat it. By recognizing the nature of glaucoma, understanding its different types, and being aware of the risk factors and symptoms, individuals can take proactive steps towards early detection and appropriate treatment.
The Evolution of Glaucoma Treatment
In the past, traditional surgical methods, such as trabeculectomy and tube shunts, were the mainstay of glaucoma treatment. While these procedures are effective in reducing intraocular pressure (IOP), they are invasive and carry a higher risk of complications. However, the field of glaucoma treatment has seen significant advancements in recent years, leading to the development of less invasive and more targeted options, including minimally invasive glaucoma surgery (MIGS).
Traditional Surgical Methods
Trabeculectomy, a widely used surgical procedure for glaucoma, involves creating a new drainage channel in the eye to improve the outflow of fluid and reduce IOP. This procedure requires making a large incision in the eye, which can result in a longer recovery time and a higher risk of complications such as infection and bleeding. Tube shunts, on the other hand, involve implanting a small tube to divert excess fluid from the eye. While effective in managing glaucoma, tube shunts also require a larger incision and carry similar risks as trabeculectomy.
Despite the success of these traditional surgical methods, the need for less invasive alternatives became evident. Patients and eye care professionals alike sought treatment options that could provide effective glaucoma management with reduced risks and shorter recovery times.
The Advent of MIGS
MIGS represents a significant breakthrough in glaucoma treatment, offering a less invasive and more targeted approach. These procedures employ micro-incisional techniques and specialized devices to bypass or enhance the eye’s natural drainage system, thus reducing IOP. Unlike traditional surgical methods, MIGS procedures can be performed through small incisions, resulting in minimal trauma to the eye and faster recovery times.
One of the advantages of MIGS is its compatibility with cataract surgery. Many glaucoma patients also have cataracts, and combining MIGS with cataract surgery allows for the treatment of both conditions simultaneously. This approach not only reduces the number of surgeries a patient needs but also improves the overall outcomes by addressing multiple eye conditions in a single procedure.
There are several types of MIGS procedures available, each with its own unique approach to reducing IOP. Some procedures involve creating a bypass to improve fluid outflow, while others enhance the eye’s natural drainage system. The specific procedure chosen depends on the patient’s individual needs and the severity of their glaucoma.
Overall, MIGS has revolutionized the field of glaucoma treatment by providing a less invasive and more targeted option for patients. With ongoing advancements in technology and surgical techniques, the future of glaucoma management looks promising, offering improved outcomes and quality of life for those affected by this sight-threatening condition.
The Science Behind MIGS
To understand the benefits of MIGS (Minimally Invasive Glaucoma Surgery), it’s important to grasp the surgical process and the role of micro-incisional techniques in glaucoma treatment. Glaucoma, a group of eye conditions that damage the optic nerve, is a leading cause of blindness worldwide. MIGS procedures offer a promising solution for patients with glaucoma, aiming to lower intraocular pressure (IOP) and minimize disease progression.
The Surgical Process
MIGS procedures are typically performed under local anesthesia on an outpatient basis, making them more convenient and less invasive than traditional glaucoma surgeries. After making a small incision, usually less than 2mm in size, the surgeon enters the eye with precision and care. The use of microscopic tools and specialized devices allows for a meticulous approach to create a new drainage pathway or modify existing ones.
By enhancing the eye’s natural drainage system, MIGS procedures help to improve the outflow of aqueous humor, the fluid inside the eye. This reduction in fluid pressure helps to alleviate the strain on the optic nerve, which is crucial in preventing further damage and preserving vision. The surgeon’s skill and expertise play a vital role in ensuring the success of the procedure and optimizing patient outcomes.
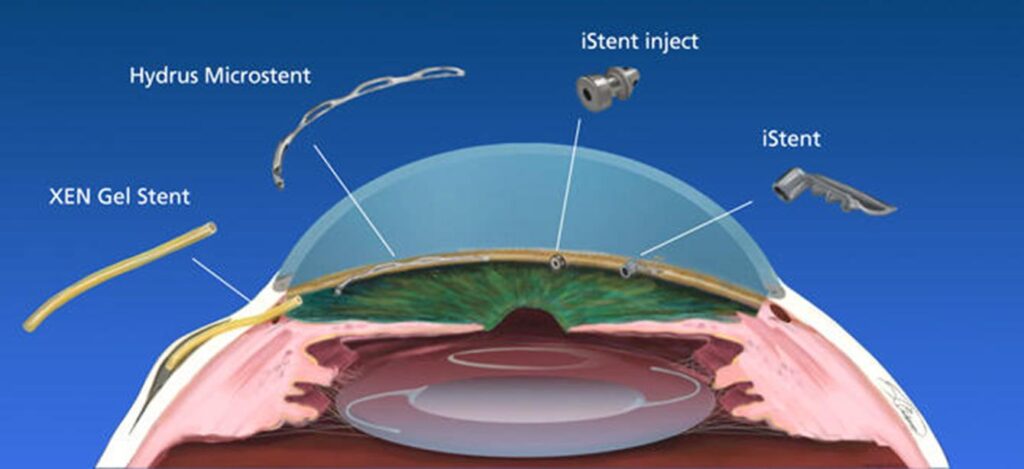
The Role of Micro-Incisional Techniques
Micro-incisional techniques are central to MIGS procedures, setting them apart from more invasive glaucoma surgeries. These techniques involve making small incisions, typically less than 2mm in size, to minimize trauma to the surrounding tissues and promote faster healing. The use of micro-incisions allows for a more precise and controlled surgery, reducing the risk of complications and improving patient outcomes.
During the procedure, the surgeon carefully navigates through the eye’s delicate structures, guided by high-resolution imaging systems. The micro-incisions provide access to the targeted areas without causing significant disruption to the surrounding tissues. This approach not only reduces the risk of bleeding and infection but also enhances the overall safety profile of MIGS procedures.
Furthermore, the smaller incisions result in minimal scarring, leading to better cosmetic outcomes. Patients often appreciate the aesthetic benefits of MIGS, as the incisions are barely noticeable and tend to heal quickly. The reduced postoperative discomfort and faster recovery time associated with micro-incisional techniques contribute to the overall patient satisfaction and improve the quality of life during the healing process.
In addition to their role in glaucoma treatment, micro-incisional techniques have revolutionized various other ophthalmic procedures. They have been widely adopted in cataract surgery, allowing for smaller incisions and quicker visual recovery. The advancements in micro-incisional techniques continue to drive innovation in the field of ophthalmology, enabling surgeons to perform intricate procedures with greater precision and patient comfort.
In conclusion, MIGS procedures leverage the science of micro-incisional techniques to provide a less invasive and more precise approach to glaucoma treatment. By utilizing small incisions and specialized tools, surgeons can enhance the eye’s natural drainage system, reduce intraocular pressure, and potentially halt the progression of glaucoma. The continuous advancements in micro-incisional techniques hold promise for further improving patient outcomes and expanding the scope of minimally invasive ophthalmic surgeries.
Benefits of MIGS
MIGS offers several advantages over traditional surgical methods, making it an attractive option for both patients and surgeons.
Reduced Recovery Time
One of the significant benefits of MIGS is the reduced recovery time compared to traditional surgeries. Since MIGS procedures are less invasive, patients often experience minimal discomfort and can resume their normal activities sooner.
Lower Risk of Complications
Traditional glaucoma surgeries carry a higher risk of complications, including infection, bleeding, and prolonged inflammation. MIGS procedures, with their micro-incisional techniques, have been shown to have a lower risk of such complications, increasing patient safety and satisfaction.
Potential Drawbacks and Limitations of MIGS
While MIGS has revolutionized glaucoma treatment, it is essential to consider its potential drawbacks and limitations.
Suitability for Different Glaucoma Stages
MIGS procedures are most effective in mild to moderate stages of glaucoma. In advanced stages, where the damage to the optic nerve is severe, more invasive surgical options may be required. It’s crucial for patients to undergo a comprehensive evaluation to determine the most appropriate treatment approach.
Long-Term Efficacy and Safety
MIGS is a relatively new field in glaucoma treatment, and its long-term efficacy and safety are still being studied. While current evidence suggests positive outcomes, more research is needed to establish its durability and effectiveness in the long run.
In Conclusion
MIGS represents a significant advancement in glaucoma treatment. Its minimally invasive nature, coupled with its potential benefits, make it an attractive option for patients and a valuable tool for surgeons. While MIGS is not suitable for all glaucoma cases, it offers new possibilities in managing the disease and preserving vision. As technologies continue to evolve, MIGS is likely to become an integral part of the comprehensive approach to glaucoma care.